Periodontal disease ( "gum disease" ) is an infection of the gum and bone supporting the teeth in the jawbone. It is the main cause of tooth loss in adults.
Gum disease is caused by dental plaque, a biofilm of bacteria that forms on teeth. If you brush your teeth thoroughly, the bacteria grows back onto the teeth within 24 hours. You need to clean your teeth twice daily.
10% of the population are genetically more susceptible. Regular cleaning and monitoring is required to prevent recurrent problems.
Periodontal disease is usually painless.
What are the warning signs?
- gum bleeds during toothbrushing
- red, swollen or tender gums
- gums receding
- bad breath
- pus discharge when pressing on gum
- Loose or drifting teeth
- food trapping between teeth
- the bite has changed over recent months
- denture is now loose
What are some of the ways to treat gum disease?
It can take many months to change problems that have built up over years.
We employ a step by step strategy to
ensure you have the time to understand your own requirements and the
dentist can evaluate progress.
Behaviour change: if you cannot change
the way you look after your teeth, the problem will not go away. It
is what you do on a daily basis that is important. So...you must
clean your teeth the way we want you to, not the way you have always
done it.
Oral hygiene instruction: Don't worry
most people were never taught so it is our job to ensure you become
an expert.
Scaling and polish
above the gum line
Medical history
Smoking is a risk factor and we will advise on stopping
smoking.
Genetics: some patients develop very
advanced periodontal disease and can loose teeth from a young age.
Diabetes if uncontrolled can contribute
to periodontal disease
Removal of defective fillings to allow
access for you to clean your teeth properly.
Cleaning below the gum line: this should
only be done when there is a recorded period where you have
demonstrated a high standard of oral hygiene. The gums are also
starting to settle down with less bleeding and the teeth appear more
firm. The dentist or hygienist at this stage will use local
anaesthetic to numb the teeth and clean the remaining hard calculus
deposits on the root surfaces. This process may take a few visits or
sometimes two long appointments.
Review:
Periodontitis affected clients are kept under regular review and
maintenance. This is a necessary behaviour change. It is no good
getting this far and disappearing again until the problems restart.
Mobile teeth: if teeth are still mobile
but healthy, they can be splinted for comfort.
Persistent problems: It may be that some teeth fail to respond to normal cleaning. Gum access surgery may be indicated. This is discussed on an individual patient basis. Using various surgical techniques, the dentist lifts the gum away to reach areas that require the removal of tartar and plaque, which cause chronic infection and delay healing. The tooth root is cleaned and smoothed. The gums are sutured back into place or into a new position that will be easier to keep clean at home.
Guided tissue
regeneration: some bone defects may be amenable to GTR. This
is an advanced procedure and involves bone augmentation to regain
lost bone support.
Antibiotics may be prescribed in
selected cases to help control the growth of bacteria deep in the
tissues. This may be required to encourage normal healing.
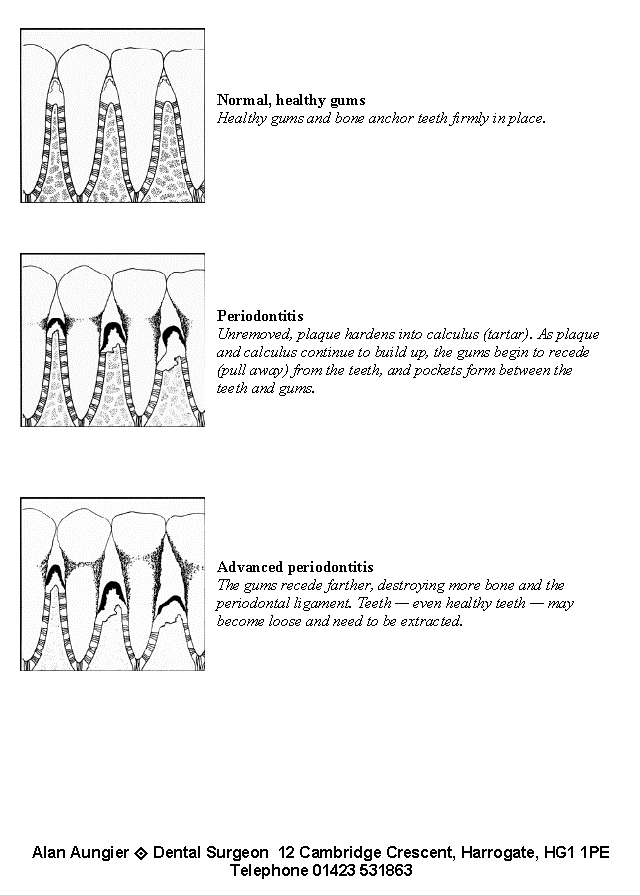
How does Periodontal disease progress if left untreated?